Metastasis — the spreading of cancer to other regions in the body — is responsible for 90% of cancer deaths. Yet not much is known about what makes cancer cells capable of metastasizing. Now a major study from investigators at the Sloan Kettering Institute concludes that metastasis-initiating cells employ a devilish trick to spread: They co-opt the body’s natural wound-healing abilities.
The new findings, published January 13 in the inaugural issue of the journal Nature Cancer, provide a novel framework for thinking about metastasis and how to treat it.
“We now understand metastasis as the regeneration of the wrong tissue — the tumor — in the wrong place — distant vital organs,” says Joan Massagué, Director of the Sloan Kettering Institute and the corresponding author on the paper. “This is not just a metaphor. It is literally true in molecular and physiological terms.”
There were previously clues that cancers might make use of wound-healing pathways to support their growth. Back in the 1980s, researcher Harold Dvorak dubbed tumors “wounds that do not heal.” But the new findings present the first detailed picture of how this process works on the level of cells and molecules — and there are plenty of surprises.
A Long and Difficult Road
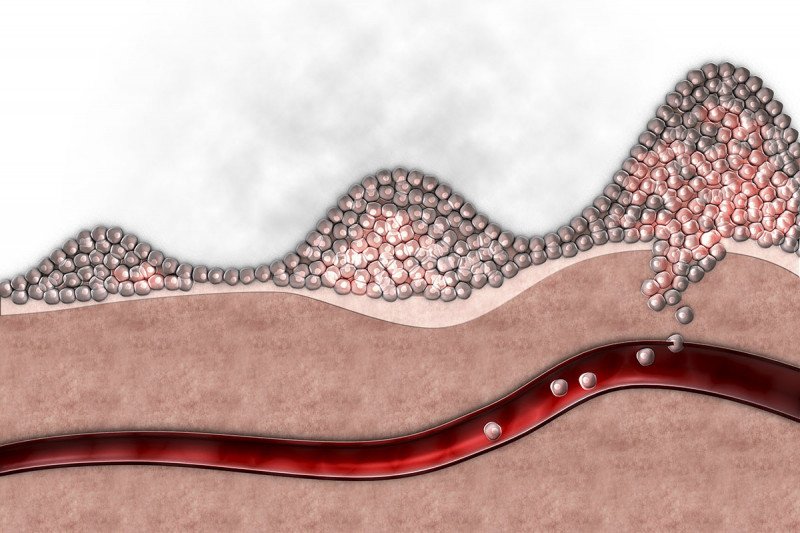
Though metastasis is deadly, it’s not something that cancer cells can do easily. To spread, cancer cells must successfully detach from their neighbors, break through tissue layers separating them from the circulation, swim or crawl to a new location in the body through blood or lymph fluid, exit these vessels, then take root and start growing in the new location.
At each step in this process, the majority of loose cancer cells die off. Fewer than 1% of all cancer cells shed from a tumor will ultimately form measurable metastases. But those that do will have proven themselves to be unusually hearty.
“Once cancer cells learn how to survive the stress of living in a foreign environment, they’re very difficult to get rid of,” says Karuna Ganesh, a physician-scientist in the Molecular Pharmacology Program at SKI and the paper’s first author. “They are a completely different entity from the tumor that they started off in.” But not, it seems, because they have different mutations.
Dr. Ganesh and her colleagues wanted to understand what enables some cells to survive this stressful journey. They homed in on a molecule called L1CAM, which previous studies from the Massagué lab had shown is necessary for numerous types of cancer cells to successfully metastasize to organs. Normal healthy tissues do not typically make L1CAM, but advanced cancers often do. Exactly what triggers the expression of L1CAM has so far been a mystery.
L1CAM as a Marker of Wound Healing
From looking at human tumor tissues under a microscope, it was clear to the researchers that dividing cells with L1CAM were more common in areas where an epithelial layer was disrupted — that is, wounded. This led the scientists to wonder whether L1CAM is required for normal wound repair, such as occurs in the intestine following colitis. Using a mouse model of colitis, they found that indeed this was the case.
Next, they wanted to know exactly what it is about the wounding process that causes cells to switch on L1CAM. To find out, they turned to a recently developed technology called tissue organoids. These three-dimensional structures are grown from human cells and in many ways resemble human organs. Working with MSK colorectal cancer surgeon Julio Garcia-Aguilar, Dr. Ganesh was able to obtain fresh samples of metastatic colorectal tumors, which she then grew in jelly until they formed three-dimensional tumor organoids.
Using these tumor organoids, she and her colleagues were able to show that simply separating cells from their neighbors was enough to trigger L1CAM production. What’s more, the organoids enabled the researchers to work out in detail the molecular signals that switch on L1CAM.
Why would metastasis-initiating cells share a marker of wound healing? Fundamentally, wounds are a breach in the integrity of the epithelial layer of our skin: Cells that are normally linked tightly to each other to form a protective barrier are suddenly separated from their neighbors. Similarly, in metastasis, cells detach from their neighbors and adopt a migratory behavior to reach new locations. The researchers suspect that the wound repair program equips both types of cells to survive this anchorless state. In the first case, it allows cells to move into the breach and make new tissues, which is a good thing; in the second, it enables metastatic cells to detach and colonize new destinations, which is very bad.
“Metastasis is wound healing gone wrong,” Dr. Ganesh says.
Models Matter
Since previous researchers had linked cancer growth to wound healing, the SKI scientists asked whether cells that produce L1CAM are necessary to initiate the growth of a primary tumor. Using a mouse model, they found — somewhat surprisingly — that they were not; tumors formed fine without it. However, these L1CAM-making cells were necessary for tumors to metastasize. This led the researchers to conclude that the stem cells that form primary tumors are different from the ones that form metastases.
Scientists are increasingly interested in cancer stem cells — the subset of cells within a tumor than can regrow a tumor. A crucial lesson from these findings is that cancer models that rely on the growth of primary tumors are not adequate for understanding metastasis — or for testing medicines that might treat it. That’s because the stem cells that generate primary tumors are fundamentally different from those that generate metastases.
The SKI scientists think that this newly identified connection between metastasis-initiating cells and wound healing will open up promising avenues of research. They are currently looking for drugs that might block L1CAM and thereby rob cancer cells of their ability to metastasize. They plan to continue collaborating with MSK colleagues to bring these insights to the patients in the clinic.
“There is such a strong translational environment at MSK,” Dr. Ganesh adds. “Everybody is eager to collaborate on work that might improve outcomes for patients with metastatic cancer.”
This work was supported by National Institutes of Health via grants P01-CA129243 (J.M.), P01-CA094060 (J.M.), P30-CA008748 (MSKCC), K08-CA230213 (K.G.), T32-CA009207 (K.G.), T32-GM007739 (K.P.O. and Y.-H.H.) and F30-CA203238 (Y.-H.H.), a Department of Defense Innovator Award W81XWH-12-0074 (J.M.), the Damon Runyon Foundation, the American Cancer Society, the American Association for Cancer Research, the Conquer Cancer Foundation, the Shulamit Katzman Foundation, Burroughs Wellcome, and the Alan and Sandra Gerry Metastasis and Tumour Ecosystems Center at MSK. Dr. Ganesh is an investigator of the Stand Up To Cancer Colorectal Cancer Dream Team. Dr. Massagué is a science advisor for and owns company stock in Scholar Rock.