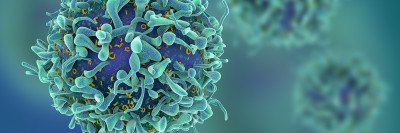
A natural killer cell (top right) attacks and kills a cancer cell (center), which blebs and spills its contents. Video courtesy of Morgan Huse.
Most people familiar with the immune system have heard of T cells. These versatile immune cells, which protect us from infections and cancer, have been the focus of immunotherapy — approaches that use the body’s immune system to fight cancer.
Lesser known, but no less important to healthy immune function, is an immune cell called a natural killer (NK) cell. These specialized fighters destroy damaged or stressed cells, including those infected with viruses and ones showing signs of genetic damage.
NK cells are experiencing something of a renaissance these days. Scientists are finding they can’t fully understand the body’s response to cancer without taking these cells into account.
In 2016, for instance, scientists at the Sloan Kettering Institute discovered that NK cells play a role in metastatic latency. This means that they help keep rogue cancer cells in check and prevent the disease from growing and spreading.
And just last month, researchers at the University of California, San Francisco (UCSF) found that the presence of NK cells in a tumor may help explain why some people respond to certain types of immunotherapy while others do not.
So what sets these Quentin Tarantino–esque cells apart from other immune cells?
Natural-Born Killers
As their name implies, natural killer cells have a special ability to kill their targets without needing to be trained. This contrasts with other immune cells, like T cells, which have to learn how to recognize danger.
NK cells have two main ways of taking out threats. One is by detecting the presence of stress signals emitted by cells in trouble, including those with genetic damage that might lead to cancer. These stress signals cue NK cells to kill them, in a kind of altruistic self-sacrifice.
“I tell my students that stressed cells put up ‘kill me’ flags,” says Joseph Sun, an immunologist in SKI and a professor at the Gerstner Sloan Kettering Graduate School of Biomedical Sciences who studies NK cells.
The other way NK cells protect us is by recognizing cells that lack identifiable markers of “self.” Each of our cells has a molecule on it called MHC that differentiates our cells from other people’s cells. NK cells are naturally equipped to kill cells that lack these self-identifying molecules, which in most cases means virally infected cells. Certain viruses have evolved to trick the cells they infect into removing MHC molecules from their surface. This allows the viruses to fly under the radar of T cells, which require MHC for their action.
Luckily, removing MHC makes the infected cells vulnerable to killing by NK cells.
Cancer cells also sometimes remove their MHC molecules, which means that T cells can’t protect us from these transformed cells, but NK cells can.
Rewriting the Textbooks
Biology textbooks usually refer to NK cells as part of the innate immune system. This is the system of immune defenses that are present from birth and are always active. Innate immune cells are good at stopping invaders at the gate, but they don’t stick around after a fight, and they don’t learn from past experience.
This description doesn’t apply very well to NK cells, it turns out. “NK cells remember, and they can persist in the body for long periods of time,” explains Dr. Sun, whose lab discovered some of these previously unrecognized properties of NK cells. “This makes them more like the T or B cells of the adaptive immune system.”
Dr. Sun discovered these adaptive qualities of NK cells while he was a postdoctoral fellow in Lewis Lanier’s lab at UCSF. “People were very skeptical at first because, for the longest time, the dogma was that NK cells are innate. Anytime you challenge what’s written in a textbook, you’re going to get some backlash from certain folks in the community,” he explains.
But over time, he says, more and more evidence in both mice and humans has supported his findings. “I think it’s far more accepted now,” he says.
It makes sense: NK cells, T cells, and B cells all develop from the same precursor cell, called a common lymphoid progenitor. They’re basically siblings.
Role of NK Cells in Immunotherapy
Scientists have begun exploring the use of NK cells in cancer immunotherapy. Some groups have equipped NK cells with chimeric antigen receptors (CARs), in the hopes that these cells will prove safer or more effective than CAR T cells, for example.
And NK cells may be playing an unacknowledged role in other types of immunotherapy. Like T cells, NK cells have immune checkpoint molecules, such as CTLA-4 and PD-1. These molecules function like brakes on immune cell activity. They are common targets for the immunotherapy drugs called checkpoint inhibitors. While T cells get most of the credit for the sometimes dramatic responses seen in people receiving these drugs, it could be that NK cells are also contributing to the effect.
“What some T cell biologists probably don’t recognize, or just happily ignore, is that you’re probably unleashing the NK cells as well,” Dr. Sun says. “They’re likely contributing to the response.”
Infection as a Model System
Dr. Sun primarily works on viral infections, rather than cancer. His lab is interested in understanding how NK cells alter their pattern of gene expression after fighting off a viral infection. They focus specifically on a virus called cytomegalovirus (CMV).
His work could help newborns and people with suppressed immune systems, who are vulnerable to CMV infection. This includes people receiving bone marrow transplants for leukemia, for example. Many people have CMV, but in healthy people, NK cells constantly keep the virus in check. When the immune system is suppressed, the virus can replicate and cause disease.
“CMV is a huge problem and can be life-threatening in immunosuppressed patients,” Dr. Sun says. “It’s made us think about ways we can try to translate what we are learning about NK cells in our lab to the clinic.”
He and his colleagues are now looking at epigenetic changes — those involving how DNA is packaged — that may shape NK cell behavior. Knowing which changes allow NK cells to remember and persist is important for making better use of them in therapy for cancer and other diseases, he says.