
When it comes to body fat, what type you have and where it’s located is just as important as how much you have. Some people who are technically overweight are perfectly healthy because of where their fat is stored — subcutaneously (under the skin) rather than viscerally (around the internal organs). And there are average-weight people who are at risk for health problems due to the fat they store around their midsection.
Moreover, not all fat is the same. Some adults have small amounts of a type of fat that is more commonly found in young infants and hibernating animals. Called brown fat, this type of fat differs from the other main type of fat — white fat — that most of us are familiar with. White fat stores excess energy while brown fat burns it to generate heat, which is why hibernating bears and newborns need it.
Research in recent years has shown that, for those lucky enough to have it, brown fat comes with certain advantages. It is associated with better cardiovascular health and lower risk of diabetes, for example. The reasons for this association are not clear, but a new study from researchers at Memorial Sloan Kettering and The Rockefeller University offers some important clues.
“The more brown fat you have, the healthier the distribution of white fat in your body,” says Andreas Wibmer, a radiologist at MSK who is the first author on the study published July 7, 2021, in the journal Cell Reports Medicine. “People with brown fat have more subcutaneous fat relative to visceral fat in their body, and this translates into lower risk of conditions like diabetes and fatty liver disease.”
The study was retrospective (meaning it was based on data collected in the past), so it’s too soon to say for sure that brown fat is causing this shift from visceral to subcutaneous fat, Dr. Wibmer explains. But the data raise the tantalizing possibility that it might be possible to improve the health of certain people with obesity by activating their brown fat.
Visualizing Fat Stores
It’s only been relatively recently that scientists have known that some individuals retain brown fat as adults — typically in the neck and shoulder region. The discovery came in part from the experience of radiologists administering PET scans to people with cancer. PET scans use a radioactive version of glucose (sugar) to measure areas where glucose is consumed at a high rate, which is often indicative of cancer.
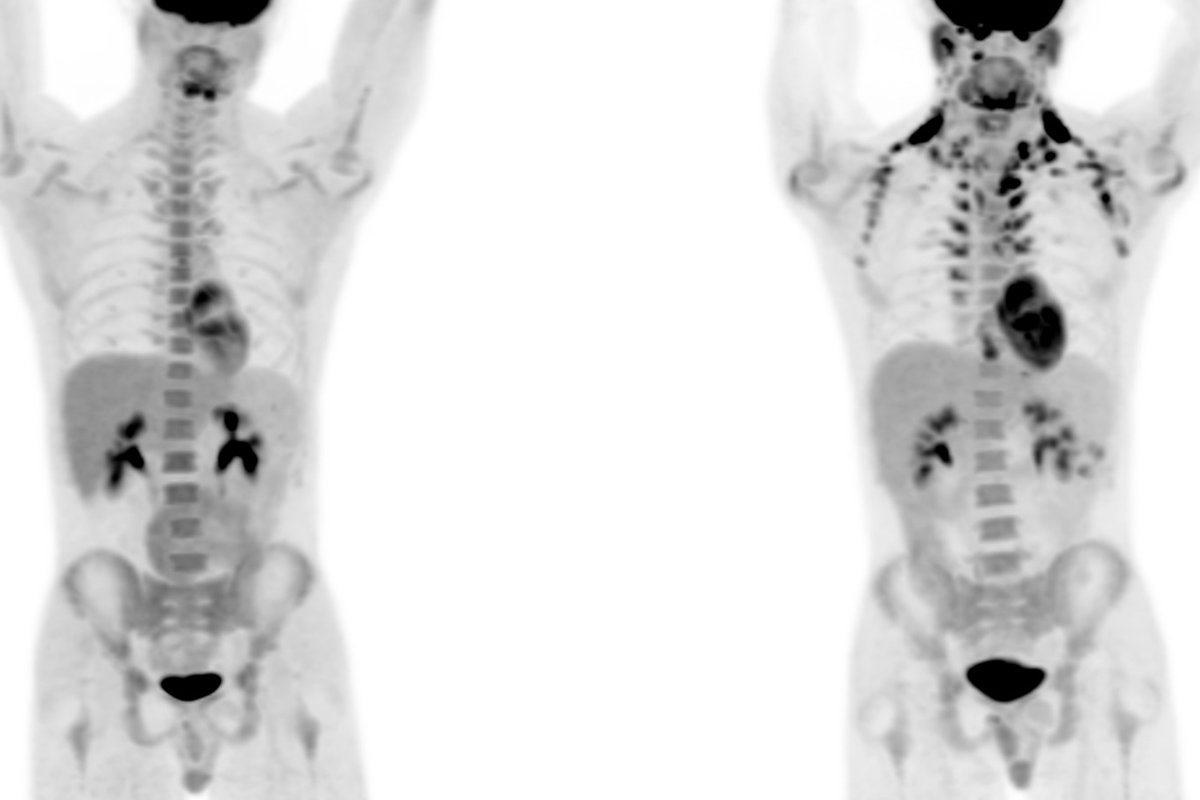
“What people saw in those scans is that the glucose went into the lower neck and shoulder area,” Dr. Wibmer says. “And that was a little scary because that’s actually where a lot of cancers form — lymphoma, for example. A few people in the nuclear medicine world hypothesized early on that it might be brown fat, and everybody said, ‘Are you kidding? Those are adults. Adults do not have brown fat.’ ”
But indeed, some do. With current PET-CT scan technology, it’s even possible to quantify just how much brown fat a person has and how active it is.
A Vast Archive
Thousands of patients at MSK undergo such scans each year, expanding an already extensive archive of data. Dr. Wibmer and his MSK colleagues, including nuclear medicine physician Heiko Schöder, realized that all of this data represented a gold mine of information. To analyze these data and look for patterns, they teamed up with Paul Cohen and Tobias Becher from Rockefeller, who are particularly interested in the biology of brown fat.
First, they grouped people into categories matched for age, gender, weight, and even time of year when the scan was taken, since ambient temperature can affect brown fat activity. Then they compared 856 people with brown fat to 846 people without it and asked how the presence of brown fat correlated with white fat distribution.
A clear pattern emerged. “We found that brown fat is associated with lower amounts of visceral fat and higher amounts of subcutaneous fat,” Dr. Wibmer says.
There was even what looked like a linear relationship: The more brown fat a person has and the more active that fat is, the better their overall fat distribution. Such a linear relationship implies that there is “a causal relationship between those two variables,” Dr. Wibmer says.
Even after statistically adjusting for body fat distribution, there were still beneficial metabolic effects associated with having brown fat. This may suggest that brown fat not only burns excess energy but also communicates directly with other organs, possibly by secreting its own hormones.
Putting Brown Fat to Work
As far as scientists know, there’s not much a person can do to alter the amount of brown fat they have. But researchers hope to find a way of boosting the activity of this fat, for example with drugs. This would benefit obese people with predominantly viscerally located fat, who seem to benefit the most from having active areas of brown fat.
“If we could only turn it on, it would give the most benefit to those who are at highest risk,” Dr. Wibmer says.
He and his colleagues are also looking at whether body fat distribution is associated with cardiovascular and metabolic health down the road in cancer survivors and will be reporting their findings soon.
- Fat comes in two main types: brown and white. Brown fat burns energy while white fat stores it.
- White fat stored viscerally (around the midsection) is more dangerous than white fat stored subcutaneously (under the skin, e.g., in the legs and buttocks).
- From studying past imaging scans of people with cancer, researchers were able to establish that having brown fat is associated with a healthier distribution of white fat in the body and lower risk of cardiovascular disease and diabetes.
This study was supported by the National Center for Advancing Translational Sciences, the National Institutes of Health (UL1TR001866), a Bernard L. Schwartz Award for physician-scientists from The Rockefeller University, the Sinsheimer Foundation, the American Diabetes Association Pathway Program Accelerator Award (1-17-ACE-17), and NIH/NCI Cancer Center Support Grant P30 CA008748.


