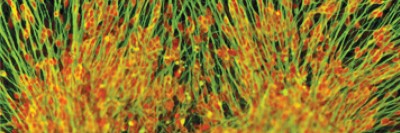
In a study published in the September 17 issue of Nature, Memorial Sloan Kettering researchers engineered stem cells from patients with familial dysautonomia (FD), a rare genetic disorder, and used them to explore the causes of the disease and to test drugs that might be effective against it. Headed by investigators Lorenz Studer, Gabsang Lee, Michel Sadelain, and Viviane Tabar, the study shows how a human disease can be modeled in a tissue culture dish — a concept with wide applications for research and drug development. [PubMed Abstract]
In patients with FD, the peripheral nervous system (PNS) fails in many of its functions, for instance in controlling heart rate and breathing. The disease is believed to be due to an inherited mutation, but its underlying mechanisms are unknown.
Using skin cells from FD patients, the investigators created genetically engineered cells called induced pluripotent stem (iPS) cells, which are similar to embryonic stem cells. The iPS cells have the same genetic makeup as the patients from whom they derive and can be made to mature into any cell type. When using them to grow artificial PNS tissue, the researchers discovered that the patient-derived iPS cells had several defects that are symptomatic of FD. For example, the cells showed signs of abnormal nerve cell development, which has also been observed in patients.
“This is the first time iPS cells have been used successfully to understand what goes wrong in a disease,” Dr. Studer explained. He and his colleagues are now using the technology to screen for candidate drugs. They have already identified one compound — a plant hormone called kinetin — that is effective in reducing FD-related defects in iPS cells.
Dr. Studer’s team has embarked on modeling a number of neurological conditions such as Parkinson’s and Alzheimer’s disease, as well as melanoma, in iPS cells. “Modeling a disease in a dish is a very powerful idea,” he said. “I think we’ve only scratched the surface of its potential.” For example, he believes the technology will prove particularly valuable for complex genetic disorders including cancers, as it could help researchers explore the behavior of an individual patient’s disease and tailor treatments accordingly.